Healthcare is rapidly evolving. Today’s hospital and health system networks require a holistic but flexible strategy to stay ahead.
Get the support you need to:
Quickly detecting and resolving issues requires standardized processes across your network. We’ll integrate our proven best practices and conduct ongoing training and development to ensure complete adoption and standardization.
Revenue cycle management automation is meant to support our solutions, not replace it. We leave the tasks that require passion to our people and automate the processes that help reduce errors, save time, and get results.
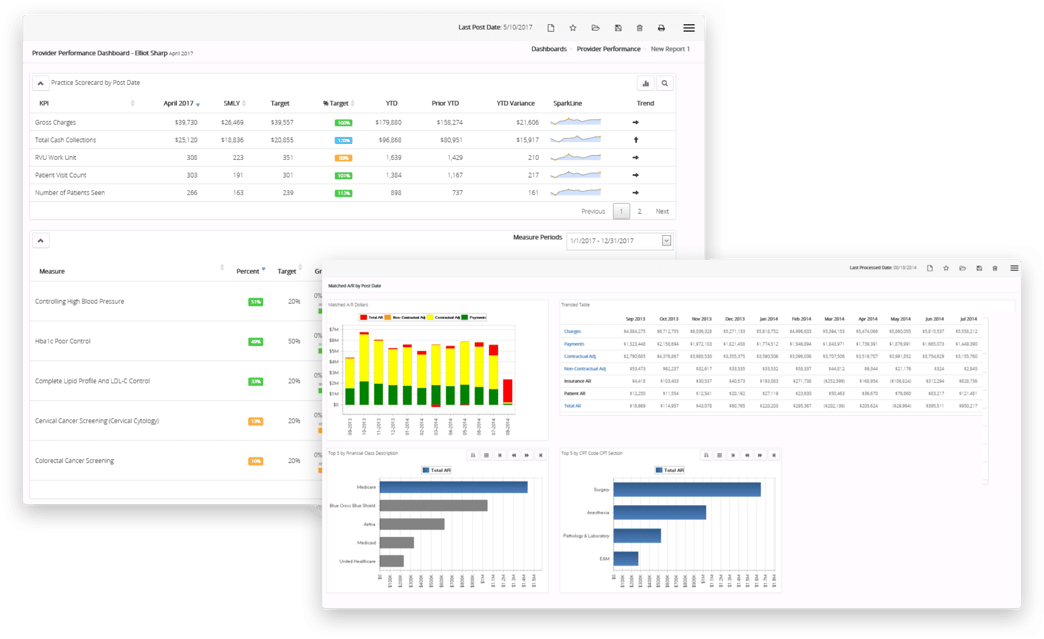
Operational and financial management insights to help hospitals and health systems measure and manage ambulatory networks. Turnkey dashboards and easy one-off reports make it easy to leverage data and analytics for strategic and tactical decision making.
We have a 25+ year history of developing and refining our controls to secure client data in an ever-changing healthcare industry. Our SOC 2 efforts and partnership with an independent third-party audit firm for HIPAA privacy and security requirements and measures help us to sustain a higher level of assurance for our customers.


Healthcare leaders are facing increased pressure to improve performance with fewer resources. Let our experts offer the extended business office support and guidance you need to improve revenue cycle management outcomes.
Revele’s Client Success Teams bring deep and diverse experience to deliver tailored consulting to help your organization succeed.
Revele's core team is the base of their support and they continue to impress our staff with their ability to address all of our concerns, even those outside the scope of billing."


©2024 Revele. All Rights Reserved.